
Importantly, early interventions aimed at emotional and behavioral disturbances are more effective when done at preschool age rather than school age ( 11). In addition to non-supportive parenting, the Adverse Childhood Experiences (ACE) score could also affect depression severity and oppositional behaviors ( 8– 10). (2014), preschool-onset depression was shown to be a predictor of MDD in later childhood. Here, preschoolers diagnosed with depression at baseline had a higher risk of developing depression at 12 and/or 24 months later in comparison to the control group ( 7). (2009), internalizing disorders such as major depressive disorder (MDD) in preschool children also show stability over time. According to a longitudinal follow-up study by Luby et al. Yet, the ones who develop serious externalizing behaviors early in life have a two- to three-fold higher risk of developing conduct disorder (CD), which is more difficult to manage and has a worse prognosis ( 4– 6). For example, oppositional defiant disorder (ODD) is a highly prevalent condition in young children (6–15%) ( 3). While many psychiatric disorders emerge in adolescence ( 2), their underpinnings can be seen much earlier. However, despite the acknowledgement of increasing pediatric mental health concerns and interventions aimed at reducing the raising suicide rates, the quality of training, implementation, and dissemination of interventions focused on the 0- to 5-year-old patient population remains inadequate. The period of 0–3 years is the most formative in human brain development (due to the critical period of synaptogenesis, pruning, and myelination) and carries the potential for lifelong consequences, both positive and negative ( 2, 3). It is estimated that as many as one in four preschool-aged children struggle with psychosocial stress and social-emotional issues, both of which may be precursors to later disease ( 1). Further research is required to tailor treatments more successfully to the child’s needs. 
At this time, it is still unclear which therapy is best indicated for which type of patients and it mostly has been driven by convenience and provider preference or training. The major challenges of clinical practice focused on young children and their families include proper diagnosis and determining the best therapeutic strategy, especially for families who have not benefited from prior interventions. These therapies have demonstrated efficacy leading to positive behavioral changes and improved parent–child interactions. 
Literature indicates that insecure or disorganized early attachments adversely affect an individual’s lifelong trajectory. Rooted in attachment theory and further supported by the premise that the quality of the child–caregiver dyad is paramount to psychological wellbeing, these therapies focus on strengthening this relationship. 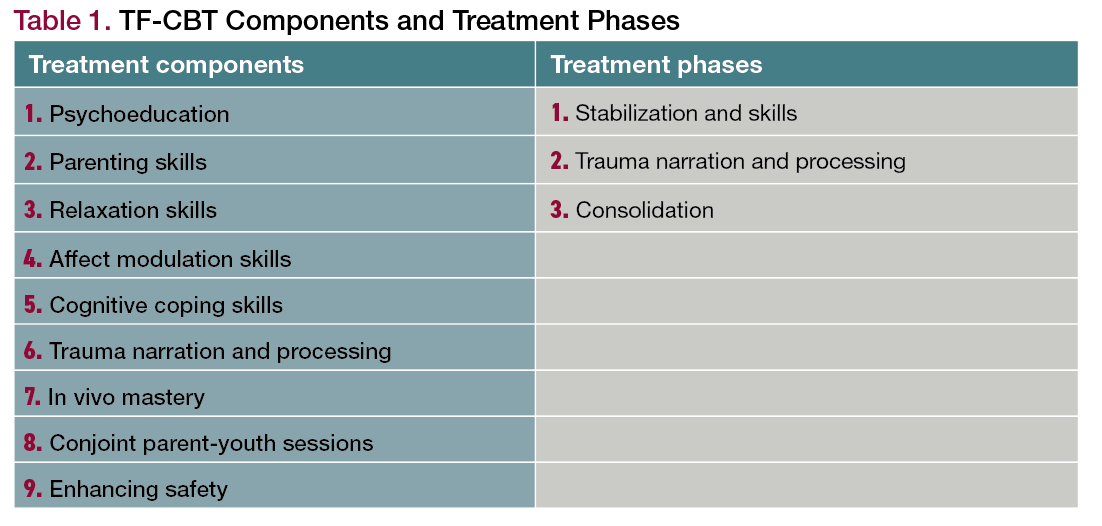
This commentary outlines indications of the four most commonly used evidence-based dyadic psychotherapies for young children: Child-Parent Psychotherapy (CPP) and Trauma-Focused Cognitive Behavioral Therapy (TF-CBT), used primarily for young children with trauma, and Parent-Child Interaction Therapy (PCIT) and Child Parent Relationship Therapy (CPRT), used mostly for children with behavioral issues. Reasons for this include limited interventions, paucity of FDA approved medications for young children, as well as the dearth of clinicians adequately trained in psychotherapeutic approaches for young children. As many as one in four preschool-aged children are estimated to struggle with psychosocial stress and social-emotional issues yet, interventions are often postponed until older ages when change is actually more difficult.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
